Clinical blood test: from a light microscope to hematological analyzers

A general clinical blood test is the most common diagnostic test that a doctor prescribes to a patient. Over the past decades, the technology of this routine, but very informative study has made a tremendous breakthrough - it has become automatic. High-tech automatic hematological analyzers came to help the laboratory diagnostics doctor, whose instrument of work was a conventional light microscope.
In this post we will tell you what exactly is happening inside the “smart machine” that sees through our blood, and why it should be trusted. We will consider the physics of processes on the example of the UniCel DxH800 hematology analyzer of the world brand Beckman Coulter. It is on this equipment that the studies ordered in the laboratory diagnostic service are performedLAB4U.RU . But in order to understand the technology of automatic blood analysis, we will understand what laboratory doctors saw under the microscope and how they interpreted this information.
Blood test parameters
So, the blood contains three types of cells:
- white blood cells that provide immune defense;
- platelets responsible for blood coagulation;
- erythrocytes transporting oxygen and carbon dioxide.
These cells are found in blood in very specific quantities. They are determined by a person’s age and state of health. Depending on the conditions in which the body is located, the bone marrow produces as many cells as the body needs. Therefore, knowing the number of a certain type of blood cells and their shape, size and other qualitative characteristics, one can confidently judge the condition and current needs of the body. It is these key parameters - the number of cells of each type, their appearance and qualitative characteristics - that make up the general clinical blood test.
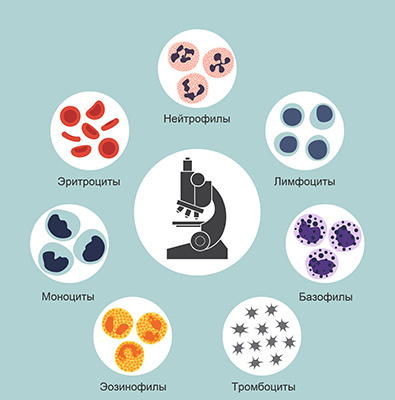
When conducting a general blood test, the number of red blood cells, platelets and white blood cells is counted. White blood cells are more complicated: there are several types of them, and each type has its own function. 5 different types of white blood cells are distinguished:
- neutrophils that neutralize mainly bacteria;
- eosinophils that neutralize antigen-antibody immune complexes;
- basophils involved in allergic reactions;
- monocytes - the main macrophages and utilizers;
- lymphocytes providing general and local immunity.
In turn, neutrophils by degree of maturity are divided into:
- stab
- segmented,
- myelocytes
- metamyelocytes.
The percentage of each type of white blood cells in their total volume is called the white blood cell formula, which has important diagnostic value. For example, the more pronounced the bacterial inflammatory process, the more neutrophils in the leukocyte formula. The presence of neutrophils of varying degrees of maturity indicates the severity of a bacterial infection. The sharper the process, the more stab neutrophils in the blood. The appearance in the blood of metamyelocytes and myelocytes indicates an extremely severe bacterial infection. For viral diseases, an increase in lymphocytes is characteristic, with allergic reactions - an increase in eosinophils.
In addition to quantitative indicators, cell morphology is extremely important. A change in their usual shape and size also indicates the presence of certain pathological processes in the body.
An important and most well-known indicator is the amount of hemoglobin in the blood, a complex protein that provides oxygen to tissues and removes carbon dioxide. The concentration of hemoglobin in the blood is the main indicator in the diagnosis of anemia.
Another important parameter is the erythrocyte sedimentation rate (ESR). In inflammatory processes, red blood cells have the property of sticking together, forming small clots. Having a larger mass, adhering red blood cells under the influence of gravity settle faster than single cells. The change in their settling rate in mm / h is a simple indicator of inflammatory processes in the body.
As it was: a scarifier, test tubes and a microscope
Blood sampling
Recall how they donated blood before: a painful puncture of a pillow with a scarifier, endless glass tubes into which precious drops of squeezed blood were collected. As a laboratory assistant, he conducted one glass over another, where there was a drop of blood, scratching the number on the glass with a simple pencil. And endless test tubes with different liquids. Now it already seems like some kind of alchemy.
Blood was taken precisely from the ring finger, for which there were quite serious reasons: the anatomy of this finger is such that its injury gives a minimal risk of sepsis in case of infection of the wound. Blood sampling from a vein was considered much more dangerous. Therefore, the analysis of venous blood was not routine, but was prescribed as necessary, and mainly in hospitals.
It should be noted that already at the stage of the fence, significant errors began. For example, different skin thicknesses give different injection depths, along with blood, tissue fluid gets into the tube - hence the change in blood concentration, in addition, blood pressure could break down when pressure was applied to the finger.
Remember the row of tubes where the blood collected from the finger was placed? To count different cells, different tubes were really needed. For red blood cells - with saline, for white blood cells - with a solution of acetic acid, where the red blood cells were dissolved, for the determination of hemoglobin - with a solution of hydrochloric acid. A separate capillary was used to determine ESR. And at the last stage, a smear was made on the glass for subsequent counting of the leukocyte formula.
Blood test under the microscope
To count the cells under a microscope in laboratory practice, a special optical device was used, proposed back in the 19th century by a Russian doctor, whose name this device was named - Goryaev’s camera. It made it possible to determine the number of cells in a given microvolume of the liquid and was a thick glass slide with a rectangular recess (camera). A microscopic grid was applied to it. From above, Goryaev’s camera was covered with a thin coverslip.
This grid consisted of 225 large squares, 25 of which were divided into 16 small squares. Red blood cells were counted in small striated squares located on the diagonal of Goryaev’s chamber. Moreover, there was a certain rule for counting cells that lie on the border of the square. The calculation of the number of red blood cells in a liter of blood was carried out according to the formula, based on the dilution of blood and the number of squares in the grid. After mathematical reductions, it was enough to multiply the calculated number of cells in the chamber by 10 to the 12th degree and add them to the analysis form.
White blood cells were counted here, but they already used large squares of the grid, since white blood cells are a thousand times larger than red blood cells. After counting the white blood cells, their number was multiplied by 10 to the 9th power and added to the form. In an experienced laboratory assistant, cell counting took an average of 3-5 minutes.
Platelet counting methods in Goryaev’s cell were very laborious due to the small size of this type of cell. Their quantity was estimated only on the basis of a stained blood smear, and the process itself was also very laborious. Therefore, as a rule, the platelet count was calculated only at the special request of the doctor.
The leukocyte formula , that is, the percentage of leukocytes of each type in their total number, could only be determined by a doctor - according to the results of a study of blood smears on glasses.

By visually determining the various types of white blood cells in the field of view by the shape of their nucleus, the doctor counted the cells of each type and their total number. Having counted 100 in total, he received the required percentage ratio of each type of cell. To simplify the calculation, special counters with separate keys for each type of cell were used.
It is noteworthy that such an important parameter as hemoglobin was determined by the laboratory assistant visually (!) By the color of hemolyzed blood in a test tube with hydrochloric acid. The method was based on the conversion of hemoglobin to brown hydrochloric hematin, the color intensity of which is proportional to the hemoglobin content. The resulting hematin hydrochloride solution was diluted with water to the color of a standard corresponding to a known hemoglobin concentration. In general, the last century
How it became: vacuum containers and hematology analyzers
To begin with, the technology for blood sampling has now completely changed. Scarifiers and glass capillaries with test tubes were replaced by vacuum containers. The blood sampling systems used now are less traumatic, the process is completely unified, which significantly reduced the percentage of errors at this stage. Vacuum tubes containing preservatives and anticoagulants allow you to save and transport blood from the sampling point to the laboratory. Thanks to the advent of new technology, it became possible to take tests as conveniently as possible - anytime, anywhere.

At first glance, it seems impossible to automate such a complex process as the identification of blood cells and their counting. But, as usual, everything ingenious is simple. An automatic blood test is based on fundamental physical laws. The technology of automatic cell counting was patented back in 1953 by the Americans Joseph and Wallace Culter. It is their name that stands in the name of the world brand of hematological equipment Bekman & Coulter.
Cell counting
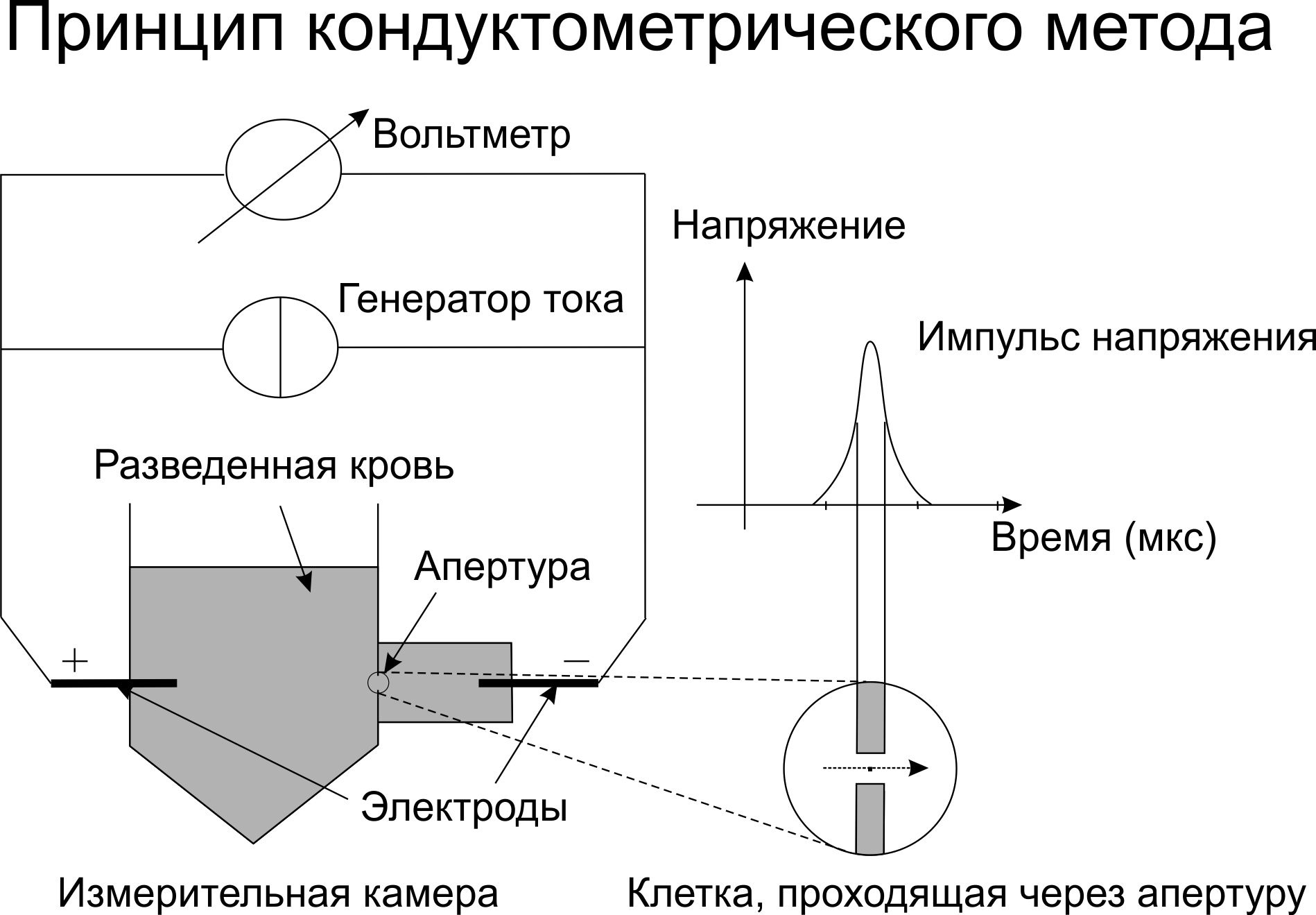
The aperture-impedance method (Coulter's method or conductometric method) is based on counting the number and evaluating the nature of the pulses that occur when a cell passes through a small diameter hole (aperture), on both sides of which there are two electrodes. When a cell passes through a channel filled with an electrolyte, resistance to electric current increases. Each passage of the cell is accompanied by the appearance of an electrical impulse. To find out what the concentration of cells is, it is necessary to pass a certain sample volume through the channel and count the number of pulses that have appeared. The only limitation is that the concentration of the sample must ensure that only one cell passes through the aperture at any given time.
Over the past 60 years, the technology of automatic hematological analysis has come a long way. Initially, these were simple cell counters that determined 8-10 parameters: the number of red blood cells (RBC), the number of leukocytes (WBC), hemoglobin (Hb) and several calculated ones. These were the first-class analyzers .
The second class of analyzers already determined up to 20 different blood parameters. They are significantly higher in leukocyte differentiation and are able to isolate populations of granulocytes (eosinophils + neutrophils + basophils), lymphocytes and an integrated population of medium cells, which included monocytes, eosinophils, basophils and plasma cells. Such a differentiation of leukocytes was successfully used in the examination of healthy people.
The most technologically advanced and innovative analyzers today are third-class machines that determine up to hundreds of different parameters, perform extensive differentiation of cells, including maturity, analyze their morphology and signal to the laboratory doctor about the detection of pathology. Third-class machines, as a rule, are also equipped with automatic smear preparation systems (including their coloring) and image display on the monitor screen. Such advanced hematological systems include BeckmanCoulter equipment, in particular the UniCel DxH 800 cell analysis system .

Modern BeckmanCoulter devices use multi-parameter flow cytometry based on the patented technology VCS (Volume-Conductivity-Scatter). VCS technology involves the estimation of cell volume, its electrical conductivity and light scattering.
The first parameter - cell volume - is measured using the Culter principle based on the assessment of resistance when a cell passes through an aperture at constant current. The magnitude and density of the cell nucleus, as well as its internal composition, is determined by measuring its electrical conductivity in alternating current of high frequency. Scattering of laser light from different angles provides information on the structure of the cell surface, the granularity of the cytoplasm, and the morphology of the cell nucleus.
The data obtained through three channels are combined and analyzed. As a result, the cells are distributed into clusters, including a division according to the degree of maturity of red blood cells and white blood cells (neutrophils). Based on the obtained measurements of these three dimensions, many hematological parameters are determined - up to 30 for diagnostic purposes, more than 20 for research purposes and more than one hundred specific calculated parameters for highly specialized cytological studies. Data is visualized in 2D and 3D formats. The laboratory assistant working with the BackmanCoulter hematology analyzer sees the results of the analysis on the monitor in approximately the following form:
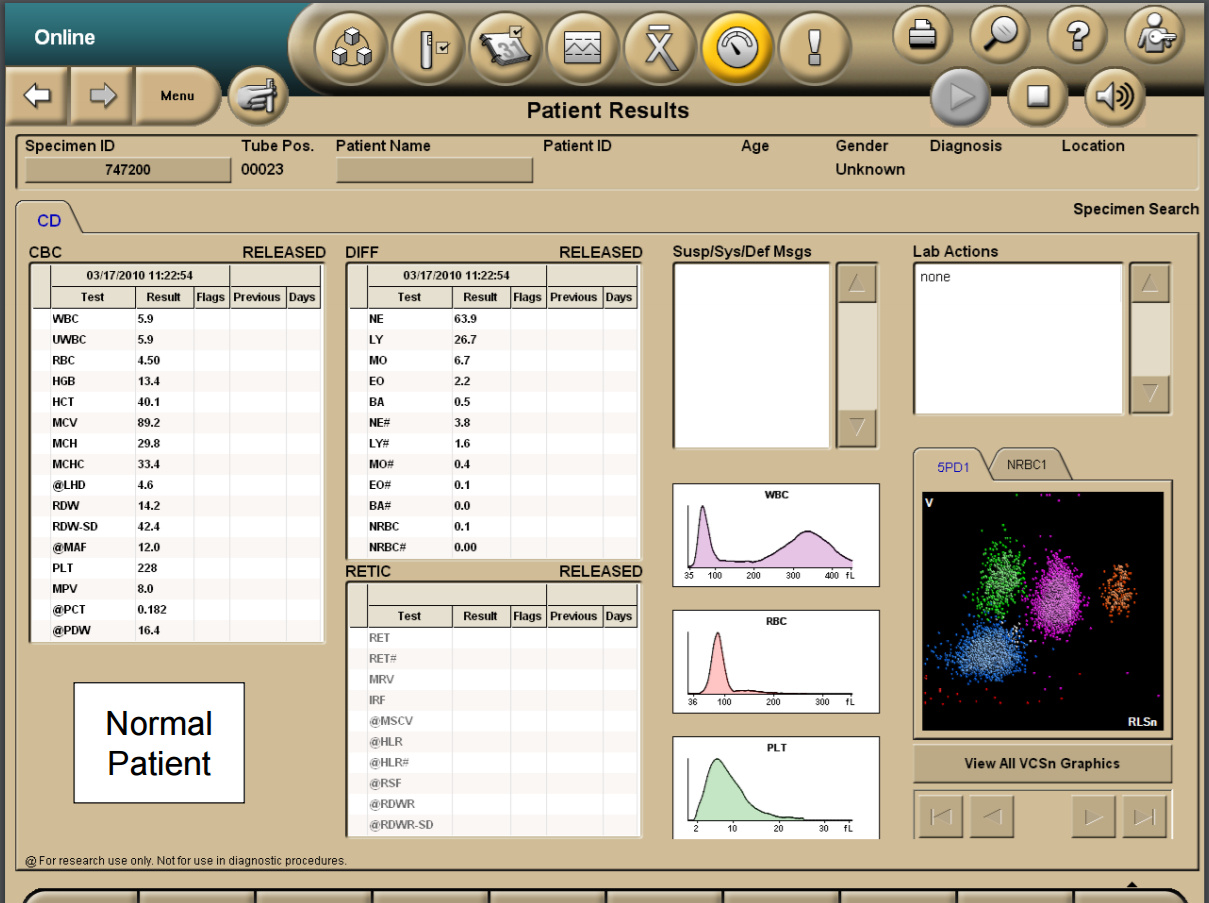
And then it makes a decision - whether they need to be verified or not.
Needless to say, the information content and accuracy of modern automatic analysis are many times higher than manual? The productivity of machines of this class is about hundreds of samples per hour when analyzing thousands of cells in a sample. Recall that under a smear microscopy, the doctor analyzed only 100 cells!
However, despite these impressive results, it is precisely microscopy that still remains the “gold standard” of diagnosis. In particular, when the apparatus reveals pathological cell morphology, the sample is analyzed manually under a microscope. When examining patients with hematological diseases, microscopy of a stained blood smear is carried out only manually by an experienced hematologist. That is how, manually, in addition to automatic cell counting, the leukocyte formula is evaluated in all children's blood tests for orders made using the online laboratory service LAB4U.RU.
Instead of a resume
Technologies of automated hematological analysis continue to develop rapidly. Essentially, they have already replaced microscopy when performing routine prophylactic analyzes, leaving it for particularly significant situations. We have in mind children's analyzes, analyzes of people with confirmed diseases, especially hematological ones. However, in the foreseeable future and in this area of laboratory diagnostics, doctors will receive devices that can independently perform morphological analysis of cells using neural networks. Reducing the burden on doctors, they will at the same time increase the requirements for their qualifications, since only atypical and pathological conditions of cells will remain in the decision-making area by a person.
The number of informative parameters of a blood test, which has increased many times over, raises the requirements for professional qualifications and for a clinician who needs to analyze combinations of parameter mass values for diagnostic purposes. To the aid of doctors of this front are expert systems that, using the data of the analyzer, provide recommendations for further examination of the patient and issue a possible diagnosis. Such systems are already on the laboratory market. But this is the topic of a separate article.
