The story of one eye and 20 operations (not read impressionable), or he wanted to be a pilot, but he was not allowed into the sky
What do you think, how many operations can be done on one eye? A clinical case of one of my patients confirms that more than 20 operations of various kinds are not the limit. Although, no doubt, this case is a record for Russia and the world of ophthalmology.
In 1978, everything was trivial - there was an 18 year old boy (let's call him “A”) who wanted to become a test pilot like his father. This was hampered by weak myopia of the right eye - only minus 1, it did not interfere with life, but the future pilot needed good vision. He decided to correct the optics of one eye by keratotomy - the old “manual” correction method at the Fedorov Institute (of course, through an acquaintance), but something went wrong. This was the first operation. Then four more in Russia, then seven more - in Switzerland. He did not become a pilot, but he became an oligarch, a man who manages serious business projects, but does not control the situation with his vision.
To me, "A" got completely disappointed in the world of ophthalmology, with 10% vision, the impossibility of correction by standard methods and high intraocular pressure. And it was a young 50-year-old businessman, successful in life (this is important - because not everything went further "like that" either). So - the next eight operations are mine. And although we expected that one or two would be enough - we had to go through almost total ophthalmic surgery - all possible types of operations.
By the way, instead of keratotomy, there would be a correction of SMILE (ReLEX SMILE) or, at least, Femto-LASIK - there wouldn’t be anything to write about - it’s impossible to do anything like that!
NOT MY STORY
So, 1978 - the first operation - radial keratotomy . This is an operation to apply notches manually on the front surface of the cornea. In the 80s, its triumphal procession began - it was widespread in the USSR and in America. If the surgeon's hand trembled - the notch turned out to be a curve or, worse, a through. The middle of the cornea flattened, the optics of the eye became weaker. The number and shape of the notches were calculated by the formulas, but the accuracy was small. "A" got everything at once - the perforation and the curvature of the notch. The cornea "slipped and twisted."
The second operation is an attempt to trim the astigmatism with notches, but already tangential (longitudinal).
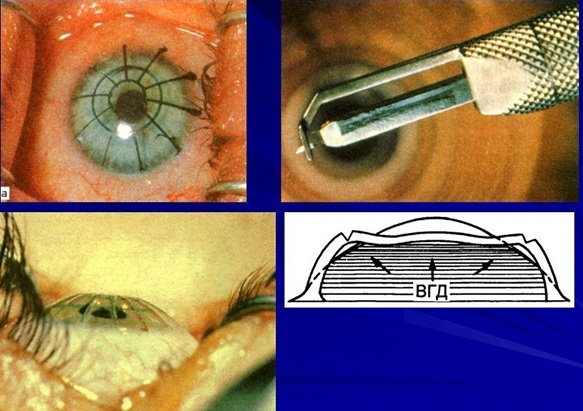
Eye in the process of keratotomy
The third operation - thermokeratoplasty - an attempt to get rid of the postoperative farsightedness obtained - by applying thermal burns of the infrared optical range laser on its periphery and the subsequent reduction of collagen fibers. Like this:

The fourth operation , 1998, is a LASIK operation . Yes, this method, which is so popular today, was pioneering at that time - they saw in it getting rid of all the problems of eye optics. The patient cut the lid from the top layer of the cornea, an excimer laser of that generation had some thickness of the stroma “evaporated” for the correction of optics, but alas - the cornea was still a curve and the vision was low. How this is done is written here .

LASIK Operation Scheme
And we remember that the cap after LASIK never-never grows - and there is a temptation to lift it again after a couple of months in order to “doze” to the goal. Thus, a fifth operation arose - the rise of the “lid” after LASIK and the excimer laser evaporation of some other thickness of the corneal stroma. The result - the cornea is critically thinned and keratectasia occurred. Keratectasia is something that is very similar to keratoconus in its course and symptoms. I wrote about it here .
Shel 2012. By this time, "A" did not become a pilot, he became a wealthy successful man and decided to be treated in Switzerland - it cost him 1 million Swiss francs. The doctor from the French part of Switzerland, who took up the treatment, decided not to touch the cornea anymore, he went the other way (he understood little of the cornea, but knew how to remove the lenses). As a result, it was decided to remove the patient's completely transparent natural lens and replace it with an artificial, complex astigmatic one, which, according to the doctor's understanding, was to compensate for the irregularities of the cornea in the right direction. The idea, in my opinion, could not be successful, since the diseased curve of the exhausted cornea was so irregular that there was no lens that could fix it.
The sixth operation iscataract phacoemulsification with the implantation of an individual pre-ordered astigmatic lens. For those who understand something in lenses - its astigmatic part was +7.5 diopters, sphere +21.0. The operation in experienced hands is 5 minutes, in the post “Implanting an Artificial Crystal Lens” you can read in detail how it is performed.
But something went wrong again - during the operation a rather terrible complication occurred in the form of a rupture of the posterior lens capsule, the surgeon left the peripheral part of his own lens and somehow managed to cope with the implantation. Rupture creates problems for the centering of the lens. The decision was made at the time of breaking the capsule, and the surgeon decided that the gap was not so large as to affect the position of the lens. Ventured and set. The idea was not the best from the very beginning: irregular astigmatism was poorly compensated, and the implant axis did not coincide with the calculated one.
The problem was that the previously ordered complex astigmatic lens could no longer be placed in a defective bag, since correct orientation would be impossible. But the lens was set, as the surgeon was hoping for a "miracle." The miracle did not happen - the optics became even more crooked.

Optics scheme with irregular astigmatism
We remember that this surgeon did not deal with the corneas, but was able to do only cataracts and change lenses. And he suggested to the patient to add another lens (!) On top of the already set, to make such a “sandwich” of them, ordering a cylinder -7.5 astigmatic with alternative axes +7.0.
The seventh operation is the implantation of this additional lens on top of the former. More precisely, he was afraid to get a lens-lens and put in its place a new one: this is a rather complicated and risky operation. As you can guess - the optics became even more crooked.
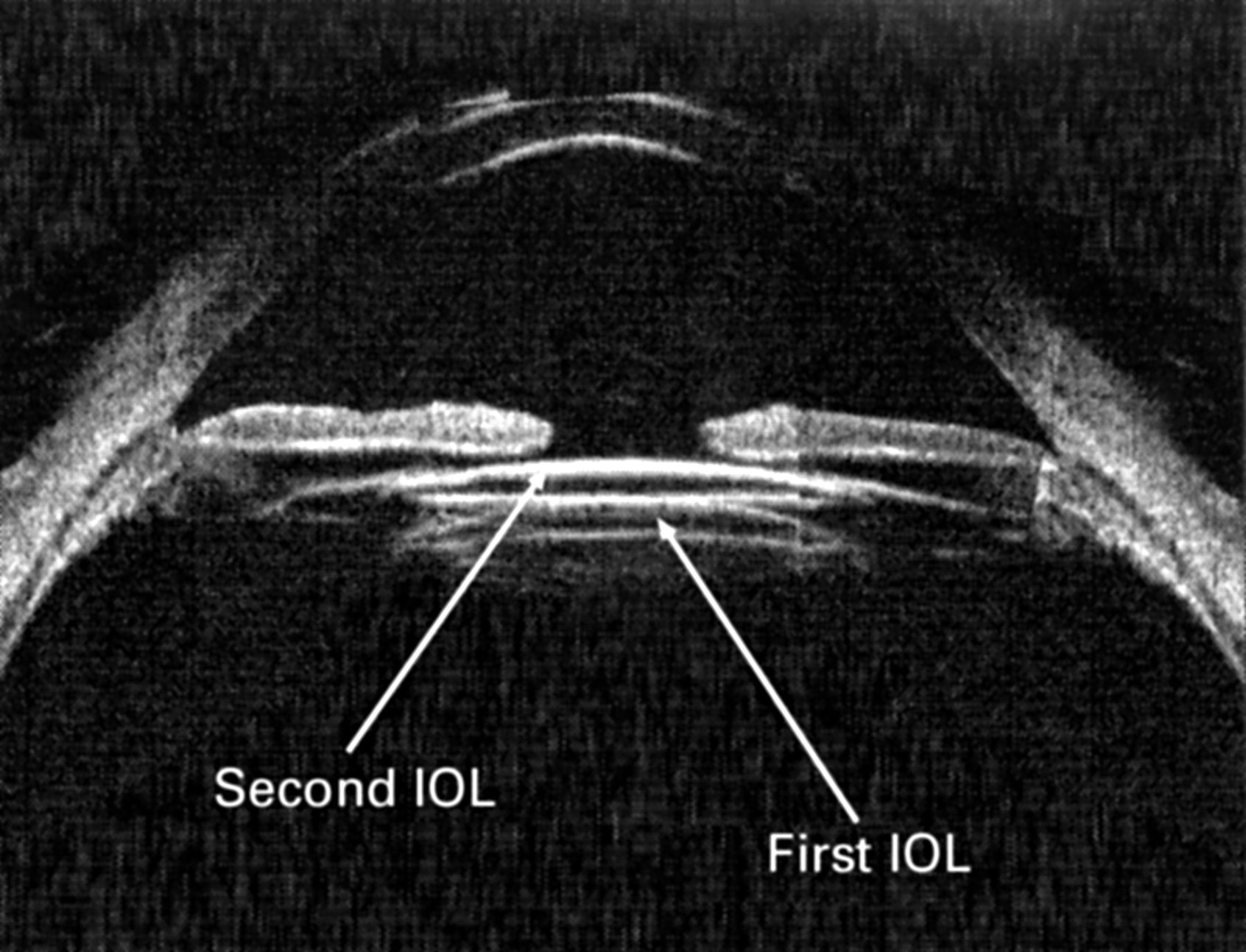
This is what ultrasound biomicroscopy with two artificial lenses in the eye looks like.
By the way, I often use such additional lenses (lenses) - they really help out in certain cases. They have a great ability - they can be rotated - rotated if necessary.

This is how clockwise or counterclockwise you can “twist” the IOL in the eye.
Thus, operation eight - in fact, this is not one, but three operations — attempts to rotate the accessory lens to bring the optics to zero. Should I write that all attempts were unsuccessful. And my colleague from the French part of Switzerland sent a patient to the German part of Switzerland to help solve the problem.
My colleague number two from the German part of Switzerland did not deal with cataracts and lenses, he was engaged only with corneas - he transplanted them and made laser corrections. And so the ninth operation happened - the surgeon honestly decided to fix the cornea in a simple safe way - tightening sutures. But they did not help.
And we remember that the specialization of this colleague is cornea transplantation. Therefore, "A" was performed tenth anniversary operation - anterior layered keratoplasty - transplanting the anterior wall of the cornea, which restored the thickness of the cornea.
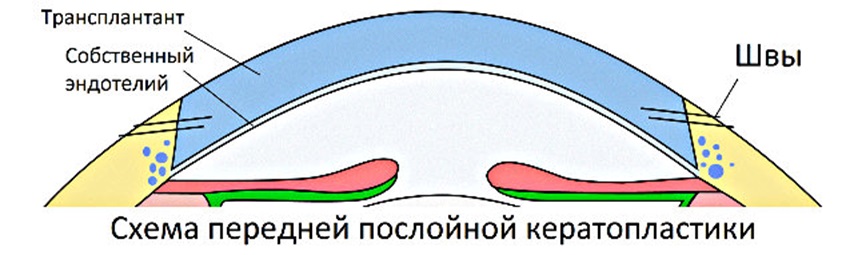
Schematically, the operation looks like this
After corneal transplantation, the optics, of course, did not become correct - after all, the transplanted cornea had the curvature and refraction of the donor (that is, the deceased person, from whom it was transplanted). To make it clear - a cornea transplant from a donor is like transferring a breast from one woman to another - when transplanting, we don’t understand the right or left eye, where the top is and where the bottom is, the curvature is not considered at all. But the surgeon expected that later he would make a femtolaser correction and correct at least the corneal component. Let me remind you that he was not an expert on lenses and he was not tormented by the question of two lenses in the eye with rather extraordinary optics.
Eleventh operation- femtoLASIK on the transplant - the 1st time. It did not work out - probably, at this time, the lenses in the eye moved and everything was squinting. How is the operation femtoLASIK written here .
The twelfth operation - re-femtoLASIK transplant. Again it did not work, and it could not happen. But the cornea thinned to 130 microns in its thinnest part (!), Although it remained fairly regular in the optical zone. This was the keratotopogram:
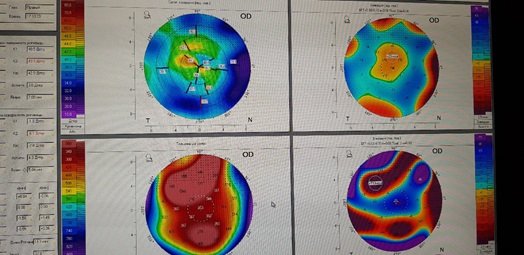

When the patient asked the Swiss surgeon - “What are we going to do next?”, He replied - “we will replant the cornea again, and then sharpen it again with a laser.”
Realizing that the circle closed, "A" returned to Moscow.
MY HISTORY
So, the patient came to me after 12 operations , with a thinned irregular cornea, the outer part of which was transplanted from the donor, low protective properties of the inner wall (endothelium), two curved lenses in the eye, high intraocular pressure - this is a complication of everything experienced and a desire to see.
Nowhere in Moscow and the world did they want to see him for several reasons:
- To solve his problem, it was necessary to start with the removal (explantation) of two curves that cause complication of the lens - no one took it up, because the rupture of the posterior capsule, which took place during the operation, made this operation extremely risky and very jeweler.
- It was difficult to calculate the optics of the new necessary lens - a vast experience of calculations and surgical intuition were needed.
- Операцию нужно было выполнять в условиях «плохой видимости», так как роговица была мутная из-за давления и рубцов.

It looked like the topography of the cornea of the patient "A"
And something had to be done. Firstly, because high intraocular pressure would destroy the optic nerve. Secondly, the patient, as you already understood, loves to be operated on. That is, so simply such people do not give up, and since they begin to fight for their vision, they finish the job.
The thirteenth operation (I don’t believe in prejudices, but still) - removing both lenses from the eye and implanting a monofocal aspheric IOL with emmetropia (we call it “zero”). The operation went great, technically managed to complete all the planned and the new lens was in the right place. I and the patient were happy - but early. There was a complication that could negate all efforts and lead to a fatal end.
As a result of multiple prior surgery, an eye reaction occurred in the form of inflammation. Not just a small one - but stormy, with a large number of cells, with thick haze and loss of vision.
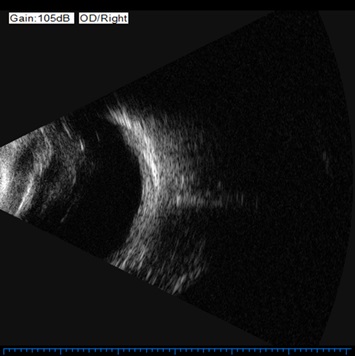
It looks like an ultrasound picture of inflammation in the posterior segment of the eye.

That was how the eye looked under a microscope.
After a couple of days, he stopped seeing objects — only light, and I stopped distinguishing anything in his eye. Unfortunately, this development is possible after numerous operations, when we have to go into the cavity of the eye. There is no vision. Consilium with colleagues did not add optimism - the general opinion that there would be one end - “eye in the basin”. It's time to give up.
It was impossible to delay. The following operation followed.
The fourteenth operation is the introduction of drugs into the anterior chamber of the eye. We took seeding for the presence of microbes (then received a negative response). In most cases it helps, but in this case the fifteenth operation was needed.- the introduction of drugs into the posterior chamber of the eye - into the vitreous cavity, since such inflammation is dangerous for the retina and can destroy it. All this, of course, against the background of general therapy.
The struggle went on day and night - we became allies in this battle. But by the third day it became clear that one could not avoid another volumetric operation.
The sixteenth operation — vitrectomy — is a deep, serious operation — removal of a turbid vitreous body, which, like a sponge, absorbs all inflammatory cells, microbes (if any) and their decay products. If you do not do this operation in time - the eye will die. The operation is very complicated, “visibility is zero”, but I managed to do it. She brought relief, a gradual improvement in the patient’s vision and a 60% vision by the end of the month. We celebrated the victory. Early.
After 2 months, "A" again had a recurrence of inflammation and vision decreased to light perception. The seventeenth operation and the eighteenth operation , the introduction of medical preparations into the vitreous cavity, have gone the same way.
And six months later, when everything calmed down, another problem was found that interfered with vision and caused distortion.
The patient saw six lines. But there were complaints of distortion. The reason for this was the formed epiretinal membrane (similar to the cellophane film covering the retina) in the center. At the same time, the new lens was excellent, and the cornea was stable.

On a CT scan, you can see the correct position of the new lens under the iris.
I do a lot of operations on the retina, including this type. But I can not say that I then wanted to do another operation. On the one hand, there are risks of recurrence of inflammation, on the other hand, there is a great temptation to help the patient, to get rid of distortions, this is impossible without surgery. We decided together what we will do!
The nineteenth operation — removal of the epiretinal and internal border membranes — looks like this: vitrectomy + work in the vitreous cavity with special tweezers for manually removing cellophane. Again, when seen bad. But everything worked out - the result of 80% of view, and the correction is all 90-100% (nevertheless, corneal astigmatism interferes).
The pressure is good, without drops. The position of the lens is normal. The cornea is still irregular, the density and quality of the endothelium is not very high. But transparency is good and allows you to see 100%.
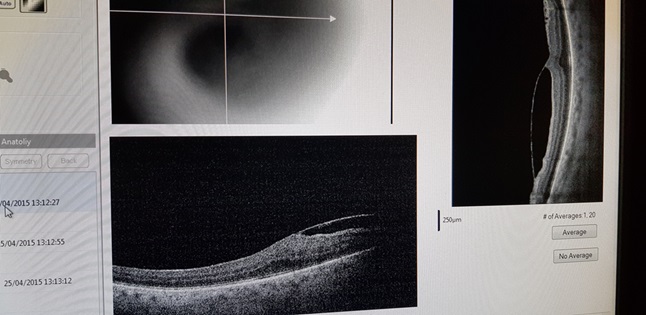
This is a tomogram of the membrane that causes distortion of the relief of the retina.
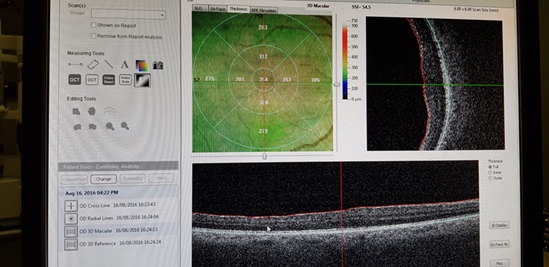
Tomogram of the retina after the 19th operation The
twentieth operation - blepharoplasty - is already aesthetic ophthalmology. The result - the patient began to see and looks younger by 10-15 years.
HAPPY END
My patient and I are best friends. He periodically asks the question: “Or maybe I still have a cornea transplanted? After all, I can see even better. ” From what I, for the time being, naturally discourage him. The eye under the microscope looks like this:

Fortunately, everything ended well. Finally : the eye is not a designer, which can be disassembled in parts and made a replacement, it has a complex structure, all structures are interconnected. Although, the further we go in the development of ophthalmology, the more we can do: something to make out, something to change.
This should be done in experienced hands, choosing specialists not of a “narrow” profile, but of those who see the eye as a whole, knowing all its departments. A clinic - with a full range of surgical operations and equipment for their operations, so that the “professional outlook” is sufficient, without limiting the choice of methods.
And also - a good doctor can fix a lot, but it's good if you turn to him right away.
Yes, the main thing is if it were our day and the patient was corrected using the methodReLEX SMILE - the story would not have taken place.
