Cute bones 3D: hyperelastic bone material for plastic skull defects

We have about 205 of them, in total they weigh about 5-6 kg and every 10 years they are completely updated at the cellular level. And there’s an idiomatic expression stating that everyone has it in the closet. This, of course, is about the skeleton and about the bones that make up it. Bone injury is one of the most common injuries in the world. Sometimes such injuries do not require bone treatment, but its replacement. Bone transplantation is associated with a number of dangers for the patient, including subsequent pain, infection, bleeding, damage to conjugated tissues, etc.
Some scientists believe that the key to successful bone transplantology lies in the use of printed bones, which will be ideal for a particular patient and will be free from defects. How did scientists print the bones, what was applied for this, and what results did the implantation operation on a rat show? We learn about this from the report of the research group. Go.
Study basis
The methods for treating bone injuries have not changed much since ancient times. Scientists even analyzed 36 Neanderthal skeletons that showed signs of fractures. Of these, only 11 treatment of these injuries can be called unsuccessful.
However, such treatment success at all times does not apply to all types of fractures. Some injuries have been successfully and without consequences treated even with sufficient modern medical equipment, knowledge and techniques.
At the moment, allografts or alloplastic materials are often used in bone transplantology.
Allotransplantation * - an organ transplant from person to person (from an individual of one species of an individual of the same species).These methods are quite advanced, but not omnipotent. Craniomaxillofacial defects (congenital, oncological or traumatic origin) are quite complex. In such cases, implants are needed that are specific to a particular patient. Therefore, they cannot be taken from the donor, but must be manufactured. In such cases, cranioplasty is used, but the implant will not have regeneration and will not grow together with other bones of the patient. Bone spongy, demineralized bone matrix, synthetic bone chips or bone putties, which fill the area of the defect, are also used. But these materials are not porous and have limited bound porosity. Because of this, surface cell migration and vascularization (vascularization) of cells are reduced, which can lead to encapsulation *rather than tissue integration. As a result, the risk of infection is greatly increased.
Encapsulation * - the formation of a capsule around a foreign body in the body.Researchers suggest using three-dimensional printing, because this method allows you to make an inexpensive implant that will ideally fit a specific defect in a particular patient.
Researchers also note that in biomedical three-dimensional printing so far there is a lack of high-performance materials that will combine ease of manufacture, use in printing and biological functionality. And this means that you need to create your own material, naturally.

Hyperelastic bone
And the name of this new material is “hyperelastic bone” (hyperelastic bone material). This osteoregenerative material is made by extrusion at room temperature of hydroxyapatite (solid, 90% of the total mass) and poly (lactic glycolic acid) (liquid, 10% of the total mass) into three-dimensional forms without the need for sintering * , curing * or other forms of physical and chemical stabilization.
Sintering * is the process of manufacturing solid and porous materials from a fine powder base at elevated temperatures and / or high pressure.
Curing * is an irreversible process of converting liquid reactive oligomers and (or) monomers into solid, non-melting and insoluble cross-linked polymers.The resulting three-dimensional printed frame has good elasticity and high absorption. In addition, the framework induces osteogenic differentiation * of bone marrow derived from human mesenchymal stem cells without the addition of osteoinductive catalysts.
Cell differentiation * - the process of forming a specialized phenotype of a cell that displays its functions. Exaggerated, the employment of cells, which previously did not have the exact profession.At the same time, the hyperelastic bone did not cause a negative immune response, became vascularized and integrated with the surrounding tissues, supporting the growth of the new bone. Another achievement is the ability to transfer transduced human fatty stem cells through a printed implant.
Next, we will take a closer look at the results of the practical test. Scientists conducted a comparative analysis of the osteoregenerative ability of hyperelastic bone and a commercial variant (autologous bone) with critical size defects in rats. But first, a little about the preparation for the experiment and how the test material and the implant were made.
Fabrication of hyperelastic bone
As we already know, the hyperelastic bone framework was made of hydroxyapatite and poly (lactic glycolic acid).

BioPlotter Printer
All samples were printed using EnvisionTEC's BioPlotter Manufacturing printer. The thickness of the sheets (5x5 cm), consisting of 5 layers of 120 μm each, amounted to a total of 0.6 mm. Next, round (8 mm in diameter) blanks were squeezed out of the sheets using a biopsy stylet. The resulting blanks were washed and sterilized.

Image # 1: implant manufacturing process.
Implantation operation
Laboratory Sprague-Dawley rats, males weighing approximately 500 grams each, were used as experimental subjects.
During the operation, the subjects were under general anesthesia (2% isoflurane / 100% oxygen). A sagittal incision (1.5 cm) was made between the lambdoid and coronal sutures to expose the skull. Using a hand drill with a trephine (a needle with a mill or a drill to form holes in dense tissues), an artificial skull defect of 8 mm in diameter was created.
Subjects were divided into 4 groups:
- 7 individuals - negative control group (without implant on the defect);
- 6 individuals - positive control group (with autologous bone as an implant);
- 6 individuals - study group No. 1 (with a framework of poly (milk-glycolic acid) as an implant);
- 10 individuals - study group No. 2 (with hyperelastic bone as an implant).
This spoiler contains a photo of the experimental during the operation (please do not look for the faint of heart, the process has been described in text form earlier).

After implantation (with or without it), the periosteum and skin were closed using a movable absorbable suture, and painkillers were administered to the experimental subjects. The subjects were kept in cells in two. Access to water and food was unlimited.
Skull samples were analyzed by cone beam computed tomography. Areas of interest were excised from the bones of the skull, placed in 70% ethanol and scanned using a micro-computer tomograph. Then, using medical imaging analysis software (Mimics Medical 19.0), scientists examined in more detail the areas of the skull where the implants were implanted.
After micro-computed tomography, the samples were cut in half for histological analysis and visualized using scanning electron microscopy. An assessment was also made of the degree of regeneration after 8 and 12 weeks.
And now we proceed directly to the results of observations.
Research results
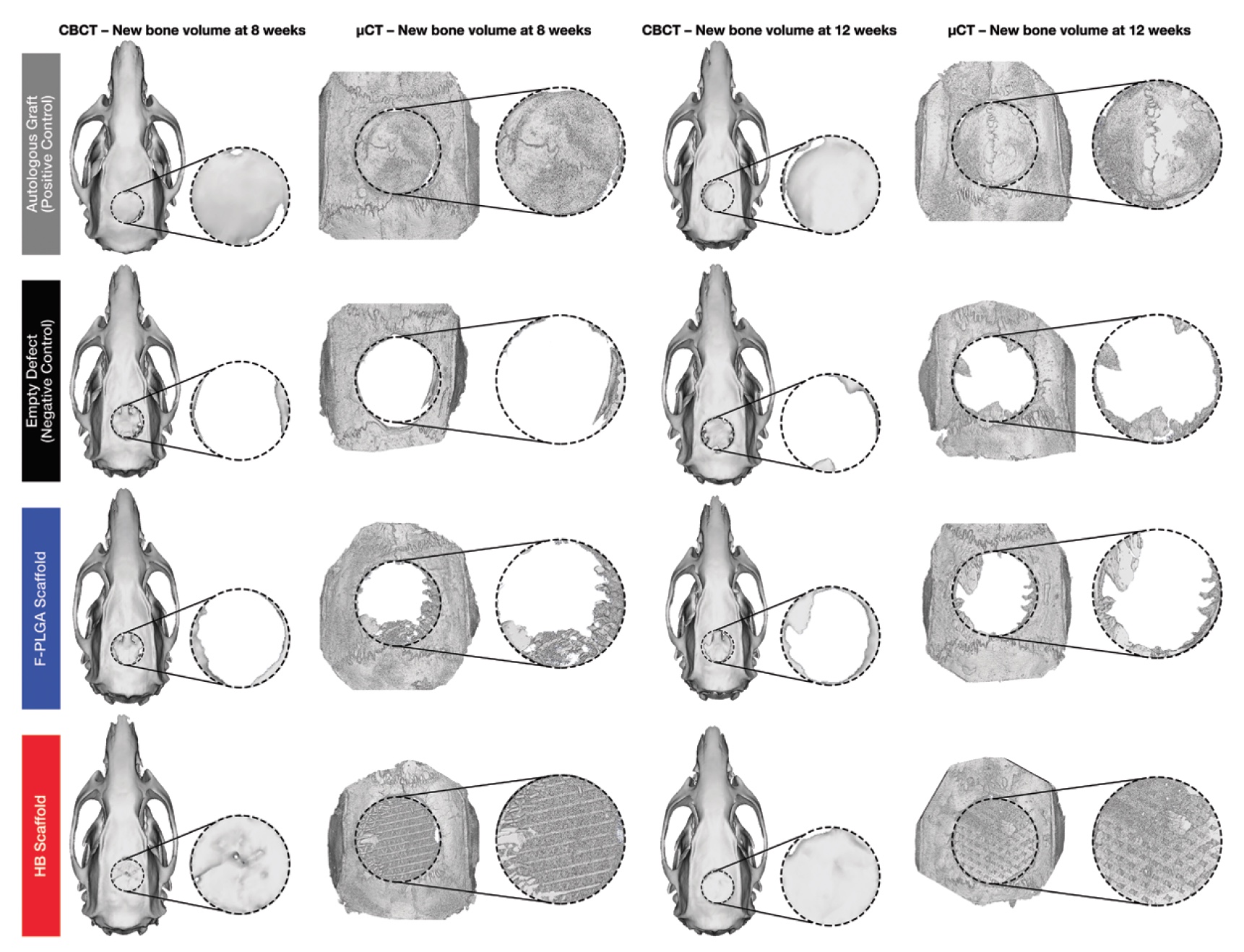
Image No. 3a: gray - with an autologous bone; black - without implant; blue - with an implant made of poly (milk-glycolic acid); red - with hyperelastic bone.
The image above ( 3a ) shows three-dimensional reconstructions of cone beam and micro-computed tomography. The amount of regenerated bone tissue was determined by the amount of mineralized bone as a fraction of the total tissue volume of interest. Bone volume per fraction of the total volume for hyperelastic bone, poly (lactic-glycolic acid) and for the negative control group were normalized relative to bone volume per fraction of the total volume for the positive control group (with autologous bone). Thus, a comparative analysis of the performance indicators of all implant options was carried out.
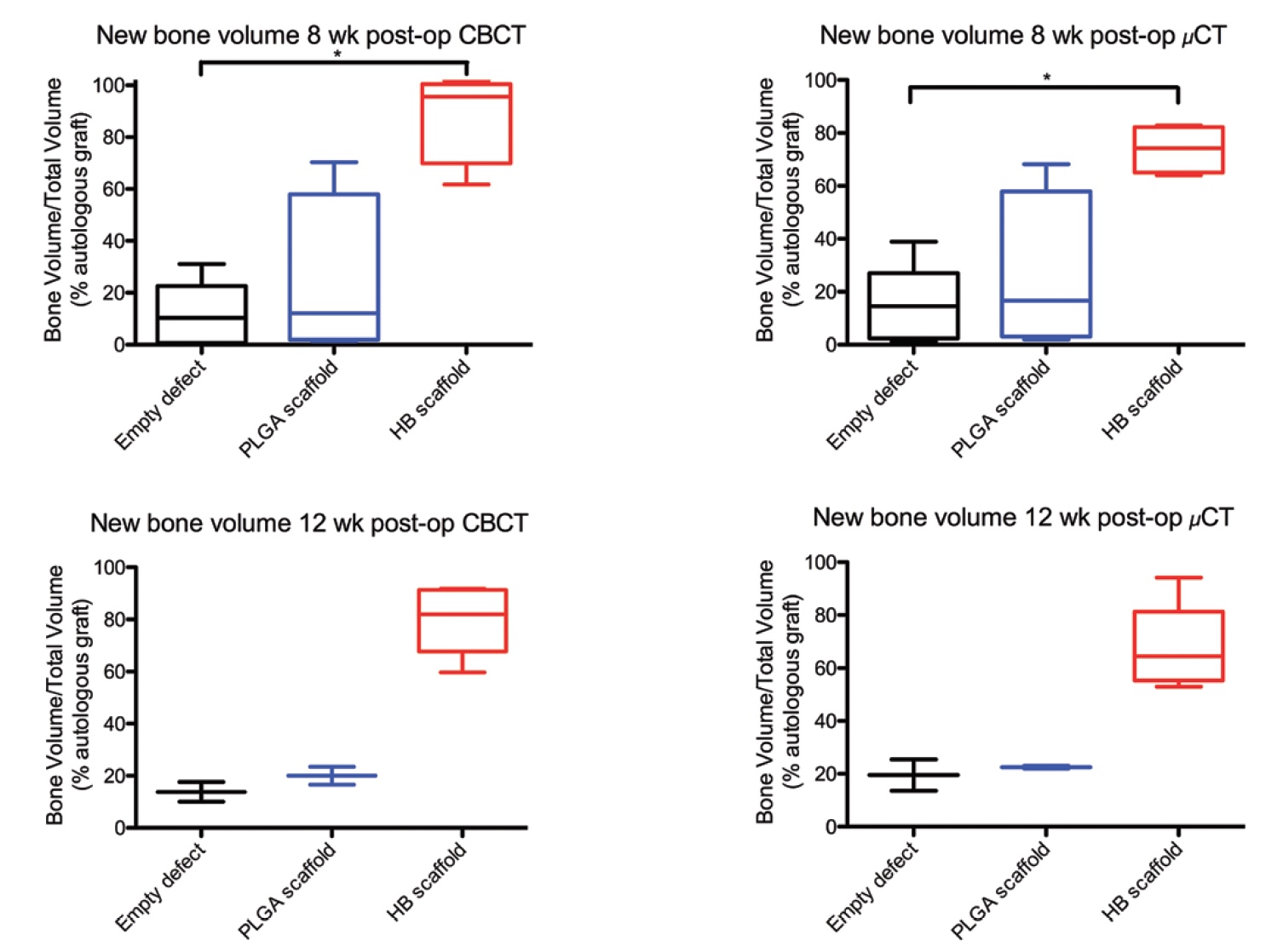
Image No. 3b
Cone beam and micro computed tomography showed an increase in the amount of mineralized bone matrix in defects treated with hyperelastic bone implants ( 3b ).
According to cone beam tomography, the volume of mineralized bone in the case of using a hyperelastic bone implant was 55.7% at 8 weeks and 57.0% at 12 weeks of observation. According to micro-computed tomography, 36.1% at week 8 and 37.1% at week 12 of observations. This is data before normalization.
After that, normalization was carried out to the indicators of the volume of mineralized bone in the case of autologous transplants. Now it became clear that the volume of regeneration using hyperelastic bone was 95.6% and 82.0% (8th and 12th week of observation) of the volume of the positive control group (with autologous bone). And micro-computed tomography yielded the following results: 74.2% and 64.5% (8th and 12th week of observations).
The use of exclusively poly (lactic-glycolic acid) as the material for implantation turned out to be quite ineffective: 16.6% and 22.5% (8th and 12th week of observation) of the positive control group. The inefficiency of this method is also confirmed by the fact that its results do not differ significantly from the results of the negative control group, which had no implants at all: 10.3% and 13.8% on cone beam tomography and 14.5% and 19.5% on micro computed tomography.
Comparison of the results of the tested new material (hyperelastic bone) with the results of the negative control group showed a difference in the volume of mineralized bone by 7.81 times at 8 weeks and 5.75 times at 12 weeks in favor of hyperelastic bone.
Thus, in terms of the volume of regeneration, the use of hyperelastic bone is practically comparable to the use of commercial implant variants with autologous bone.
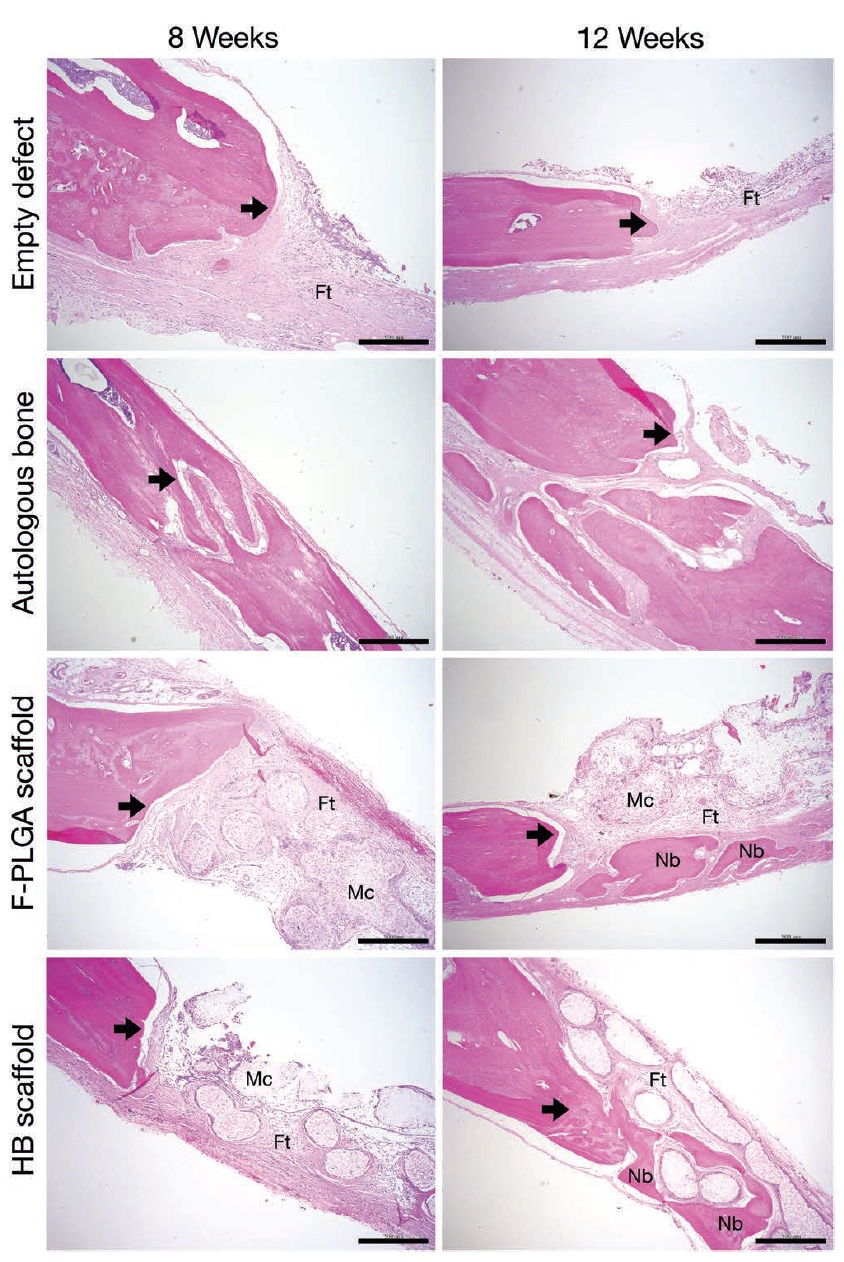
Image No. 4: arrows - defective edge; Ft - fibrous (fibrous) tissue; Mc is a membrane-cell component; Nb is the new bone.
The performed histological analysis only confirmed the data of cone beam and micro-computed tomography. Scientists identified the edges of the defects, and the formation of a new bone was specially stained with eosin for better visualization.
In the case of the negative control group, fibrous tissue was observed, but the formation of a new bone was minimal (upper row in image No. 4). Samples with poly (lactic glycolic acid) also could not boast of a large volume of newly formed bone (third row).
But the samples where hyperelastic bone was applied, on the contrary, showed the formation of mineralized bone tissue on the surface of the edges of the defects (4th row). At the 8th week of observations, at the places of defects, fibrous tissue and membrane-cell components appear inside the implant, and at the 12th week, the formation of a new bone around the elements of the implant frame begins.

Image No. 5
And finally, the analysis of SEM (scanning electron microscope) images of samples with hyperelastic bone at 12 weeks of observation showed the formation of close cellular contact of tissues with the material inside the implant.
For a more detailed acquaintance with the nuances of the study, I recommend that you look into the report of scientists .
Epilogue
In this work, scientists have demonstrated a new type of osteogenic biomaterials that allow the creation of implants for the treatment of bone defects. Scientists call the most important features of their brainchild: ease of implantation, ease of manufacture, high efficiency, low production cost and customization of the implant for a particular patient.
The hyperelastic bone is really very flexible and can take the necessary shape both during the manufacturing process and at the time of implantation, which greatly facilitates this process. Ceramic and polymer-ceramic implants cannot boast of this.
But even this is not the most important advantage. A high degree of bone regeneration and implant survival is much more important. 4 weeks after implantation, an active process of bone mineralization begins.
Scientists also note that such speed and efficiency are extremely important in the case of sufficiently large defects (as was demonstrated during practical experiments).
The use of such technology can greatly simplify the lives of both doctors and patients. The individuality of the treatment, the speed of production, implantation and a quick recovery without side effects - this is an excellent advertisement for the new technology. In the future, scientists intend to conduct several more experiments, study in more detail the regeneration process and improve their invention.
However, it is worth noting that the presence of such innovations does not mean that you can break bones left and right. So no one has canceled the safety rules.
Off-net off-top:
Yes, today is not Friday and not the time for the off-top, but I could not resist. :)
“The Corpse of the Bride” (2005, director Tim Burton)
Thank you for your attention, remain curious and have a good working week, guys. :)
Yes, today is not Friday and not the time for the off-top, but I could not resist. :)
“The Corpse of the Bride” (2005, director Tim Burton)
Thank you for your attention, remain curious and have a good working week, guys. :)
Thank you for staying with us. Do you like our articles? Want to see more interesting materials? Support us by placing an order or recommending it to your friends, a 30% discount for Habr users on a unique analogue of entry-level servers that we invented for you: The whole truth about VPS (KVM) E5-2650 v4 (6 Cores) 10GB DDR4 240GB SSD 1Gbps from $ 20 or how to divide the server? (options are available with RAID1 and RAID10, up to 24 cores and up to 40GB DDR4).
VPS (KVM) E5-2650 v4 (6 Cores) 10GB DDR4 240GB SSD 1Gbps until the summer for free when paying for a period of six months, you can order here .
Dell R730xd 2 times cheaper? Only we have 2 x Intel TetraDeca-Core Xeon 2x E5-2697v3 2.6GHz 14C 64GB DDR4 4x960GB SSD 1Gbps 100 TV from $ 199in the Netherlands! Dell R420 - 2x E5-2430 2.2Ghz 6C 128GB DDR3 2x960GB SSD 1Gbps 100TB - from $ 99! Read about How to Build Infrastructure Bldg. class using Dell R730xd E5-2650 v4 servers costing 9,000 euros for a penny?
